Dr. Erick Kazarian, MD
NYU Langone Spine Surgery — Patient Information
Scan the QR code to view this page online →
Lateral Lumbar Interbody Fusion
Lateral Lumbar Interbody Fusion (LLIF / XLIF / DLIF)
Lateral lumbar interbody fusion is a minimally invasive spine surgery that reaches the damaged disc through a small incision on your side, rather than through the back. This innovative lateral approach allows Dr. Kazarian to access the lumbar spine by gently working through the natural muscle planes of the flank, which avoids disrupting the strong back muscles and sensitive spinal nerves that a traditional posterior approach must navigate. The result is typically less muscle damage, reduced blood loss, and a faster path to recovery compared to conventional open spine fusion techniques.
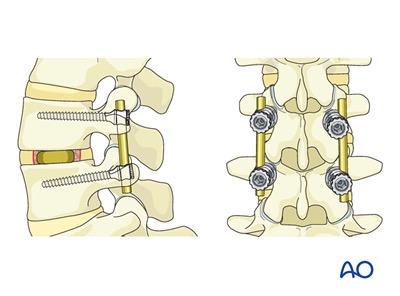
During the procedure, Dr. Kazarian removes the worn or collapsed disc and replaces it with a spacer implant that restores the natural height and alignment of the disc space. By expanding the disc height, the procedure also provides indirect decompression — meaning it relieves pressure on the spinal nerves by opening up the narrowed nerve passageways (foramina) without the need to directly manipulate the nerves. The lateral interbody portion is then supplemented with posterior percutaneous pedicle screws, which are placed through small incisions in the back using state-of-the-art robotic guidance. The robotic system creates a precise, three-dimensional map of your spine and guides each screw along a pre-planned trajectory with sub-millimeter accuracy, resulting in optimal screw placement, minimal tissue disruption, and enhanced safety.
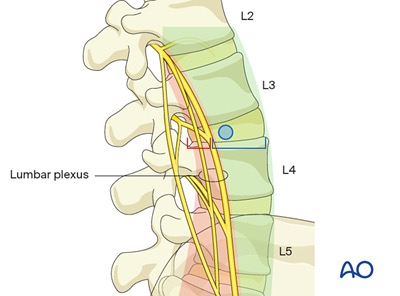
Lateral lumbar interbody fusion is most commonly used to treat degenerative disc disease, spondylolisthesis (vertebral slippage), degenerative scoliosis, and spinal stenosis in the lumbar spine. It is well suited for conditions at the L2–L5 levels and is especially helpful when multiple disc levels need to be addressed. By combining the lateral interbody technique with robotic-assisted posterior screw fixation, Dr. Kazarian leverages the latest advances in spine surgery technology to provide you with the most precise, minimally invasive procedure possible. Our surgical team will evaluate your specific condition through imaging and physical examination to determine whether this approach is the right option for you, and we will be with you every step of the way to ensure the best possible outcome.
Images & Diagrams
Pre-Operative Instructions
Carefully following these instructions before your lateral lumbar interbody fusion helps ensure a safe procedure and supports the best possible outcome. Please contact our office if you have any questions at all.
Review all current medications and supplements with Dr. Kazarian.
2 weeks before surgeryStop blood thinners (warfarin, aspirin, Plavix), NSAIDs (ibuprofen, naproxen), and herbal supplements (fish oil, vitamin E, ginkgo) as directed. GLP-1 receptor agonists (Ozempic, Wegovy, Mounjaro, Trulicity, Saxenda) must be stopped 7 days before surgery due to the risk of aspiration under anesthesia. Do not stop any medication without Dr. Kazarian's approval.
Obtain medical clearance from your primary care physician and any relevant specialists.
2-4 weeks before surgeryThis may include blood work, an EKG, and a health review. Bring clearance letters and your CPAP machine (if applicable) on surgery day.
Do not eat or drink anything after midnight the night before surgery.
After midnight the night before surgeryThis includes water, coffee, gum, and mints. You may take approved medications with a small sip of water.
The NYU perioperative team will call you the day before surgery with your arrival time.
Day of surgeryLocation: NYU Langone Kimmel Pavilion, 424 East 34th Street, Manhattan. Bring a valid photo ID, insurance card, and medication list.
Arrange for a responsible adult to drive you home and stay with you for 24-48 hours.
Arrange before surgery dayYou cannot drive after general anesthesia. Your driver should stay at the hospital during the procedure.
What to Expect on Surgery Day
Knowing what will happen before, during, and after your lateral lumbar interbody fusion can help ease any anxiety and allow you to focus on your recovery. Here is a step-by-step overview of your surgical day.
Check-In and Pre-Operative Preparation
You will arrive at the hospital approximately two hours before your scheduled procedure. Our nursing team will verify your identity, confirm the surgical level with Dr. Kazarian, and place an IV line. You will change into a hospital gown and have the opportunity to ask any remaining questions. Your anesthesiologist will review your anesthesia plan, and a neuromonitoring technician will begin placing surface electrodes on your legs and feet to monitor nerve function throughout the surgery.
Anesthesia and Lateral Positioning
You will be brought into the operating room and given general anesthesia so that you are completely asleep and comfortable during the procedure. Once the anesthesia has taken effect, the surgical team will carefully position you on your side (lateral decubitus position) with the operative side facing up. Padding and supports are used to keep your body stable and protect pressure points. This side-lying position is what gives the lateral approach its name and allows Dr. Kazarian direct access to the spine through your flank.
Lateral Interbody Fusion with Neuromonitoring
Dr. Kazarian will make a small incision on your side, typically three to five centimeters in length, and use fluoroscopic X-ray guidance to navigate to the affected disc level. Specialized retractors gently separate the psoas muscle fibers to create a corridor to the spine while real-time electromyography (EMG) neuromonitoring ensures the nearby lumbar plexus nerves are not disturbed. The damaged disc material is removed, the disc space is prepared, and a precisely sized interbody spacer filled with bone graft material is inserted.
Robotic-Guided Posterior Pedicle Screw Placement
After the interbody spacer is in place, you will be repositioned and Dr. Kazarian will place posterior percutaneous pedicle screws through small incisions in your back. This is where the procedure takes advantage of cutting-edge robotic technology: a robotic arm, guided by a three-dimensional CT-based navigation system, maps your unique spinal anatomy in real time and guides each screw along a pre-planned trajectory with remarkable precision. The robotic system allows for sub-millimeter accuracy in screw placement, which means less time in the operating room, smaller incisions, and greater confidence that every screw is in the ideal position. The screws and connecting rods lock the treated segment in place and provide the stability needed for the bone graft to fuse solidly over the coming months.
Closing the Incisions
After all hardware is in place and proper positioning is confirmed with intraoperative imaging, the retractors are carefully removed and the tissues are allowed to return to their natural positions. Both the lateral flank incision and the small posterior incisions are closed in layers with dissolvable sutures and sterile dressings are applied. In some cases, a small drain may be placed near one of the incision sites to prevent fluid buildup; this is typically removed before you are discharged.
Recovery Room
You will be taken to the post-anesthesia recovery area where nurses will closely monitor your vital signs, pain levels, and neurological status. You will be asked to wiggle your toes and move your legs to confirm nerve function. It is common to experience some soreness at the lateral flank incision and the small posterior incision sites, and some patients notice temporary numbness or tingling along the front of the thigh — this is related to the proximity of sensory nerves near the lateral surgical corridor and typically improves over time. You will then be moved to your private room, where your care team will continue to monitor your recovery. A physical therapist will help you safely sit, stand, and walk during your hospital stay. Most patients are discharged one to two days after surgery.
Risks & Potential Complications
All surgical procedures carry some degree of risk. Dr. Kazarian takes every precaution to minimize these risks, and serious complications are uncommon. Understanding the potential risks helps you make an informed decision and know what to watch for during your recovery.
Infection
There is a small risk of infection at the surgical site or deeper around the spine. Antibiotics are given before and after surgery to reduce this risk. Signs of infection include increasing redness, swelling, warmth, or drainage from the incision, as well as fever.
Blood Loss
Some blood loss is expected during spinal fusion surgery. In rare cases, significant blood loss may occur that requires a blood transfusion. Your surgical team monitors blood loss closely throughout the procedure.
Cerebrospinal Fluid Leak
The protective membrane (dura) surrounding the spinal cord and nerves may occasionally be opened during surgery, allowing spinal fluid to leak. If this occurs, it is typically repaired during the procedure. In rare cases, additional treatment may be needed after surgery.
Adjacent Segment Disease
After fusion, the spinal segments above and below the fused area may experience increased stress over time. This can lead to degeneration at those neighboring levels, potentially causing new symptoms months or years after surgery. Not everyone who has a fusion develops this condition.
Neurologic Injury
There is a small risk of injury to the spinal nerves during surgery, which could result in new or worsened numbness, tingling, weakness, or pain in the legs. In very rare cases, more significant nerve injury may occur. Dr. Kazarian uses specialized techniques and monitoring to minimize this risk.
Hardware Failure
The interbody spacer, posterior pedicle screws, rods, or other hardware used to stabilize the spine can occasionally loosen, shift, or break before the fusion has fully healed. The precision of robotic-guided screw placement helps minimize this risk by ensuring optimal screw positioning, but if hardware complications do occur, additional surgery may be needed to replace or adjust the affected components.
Nonunion (Pseudarthrosis)
In some cases, the bone may not fully fuse as expected, a condition called nonunion or pseudarthrosis. This can cause persistent or recurring pain and instability. Factors such as smoking, diabetes, and poor nutrition can increase this risk. If nonunion occurs, a revision surgery may be recommended.
Need for Additional Surgeries
While spinal fusion is often successful, there is a possibility that additional surgeries may be needed in the future. This could be due to nonunion, hardware issues, adjacent segment disease, or other factors. Dr. Kazarian will discuss your individual risk factors with you.
Femoral Nerve Injury
The lateral approach passes near the femoral nerve, which provides sensation to the front of the thigh and helps with leg movement. There is a risk of temporary or, rarely, permanent injury to this nerve, which may cause numbness or weakness in the thigh area.
Psoas Muscle Injury
The lateral approach accesses the spine through the psoas muscle on the side of the body. This muscle can be stretched or injured during the procedure, which may cause hip flexor weakness and pain when lifting the thigh, particularly in the early weeks after surgery. In most cases, these symptoms improve gradually over time.
Recovery
Recovery from lateral lumbar interbody fusion with robotic-guided posterior pedicle screws varies from patient to patient, but most people notice a significant improvement in their leg and back symptoms within the first few weeks. Because the lateral approach avoids disrupting the back muscles and the posterior screws are placed percutaneously through small incisions using robotic guidance, tissue disruption is kept to a minimum on both sides. Bone fusion typically occurs over three to six months, and your activity level will gradually increase during this time under the guidance of your surgical team. Some patients experience temporary thigh numbness or hip flexor weakness on the side of the lateral incision, which is related to the surgical approach through the psoas muscle and usually improves steadily over several weeks to months.
Prescribed Medications
| Medication | Type | Dosage | Frequency | When to Take |
|---|---|---|---|---|
| Flexeril (cyclobenzaprine) | Muscle Relaxer | 5 mg | Every 6 hours as needed | Take for moderate to severe muscle spasm or pain |
| Tylenol (acetaminophen) | Pain Reliever | 500–1000 mg | Every 6 hours as needed | Take for mild pain |
| Oxycodone | Opiate Pain Reliever | 5–10 mg | Every 4–6 hours as needed | Take for moderate to severe pain not controlled by Tylenol or NSAIDs |
Always take medications exactly as prescribed by your surgeon. Do not combine pain medications without consulting your doctor.
Early Healing and Gentle Mobilization
During the first one to two weeks, your primary focus is rest and allowing the incisions to heal. Short, frequent walks around your home are encouraged to promote circulation and prevent stiffness. You may notice soreness at the lateral flank incision as well as mild tenderness at the small posterior incision sites where the robotic-guided pedicle screws were placed. Some patients also experience temporary numbness along the front of the thigh or mild hip flexor weakness when lifting the leg. These symptoms typically begin to improve within the first few weeks.
- No bending, lifting, or twisting (BLT restrictions)
- Do not lift anything heavier than 5 to 10 pounds
- No driving until cleared by Dr. Kazarian
- Avoid prolonged sitting for more than 20 to 30 minutes at a time
- No soaking in bathtubs, pools, or hot tubs until incision is fully healed
Increasing Activity and Physical Therapy
As your incision heals and your comfort improves, you will gradually increase your walking distance and duration. Dr. Kazarian may clear you to begin a structured physical therapy program focused on core stabilization, gentle stretching, and hip flexor strengthening. Many patients begin to feel a meaningful reduction in their pre-operative leg pain and back pain during this phase. If a lumbar brace was prescribed, Dr. Kazarian will advise when it is appropriate to begin weaning off of it.
- Continue to avoid heavy lifting (nothing over 10 to 15 pounds)
- No high-impact activities such as running or jumping
- Follow your physical therapist's exercise program closely
- Avoid prolonged sitting beyond 30 to 45 minutes without standing and walking
Progressing Strength and Returning to Daily Activities
By six to twelve weeks, most patients have returned to many of their normal daily activities, including light household tasks, desk work, and driving (once cleared by Dr. Kazarian). Physical therapy progresses to include more active strengthening, flexibility exercises, and functional movement training. Any residual thigh numbness or hip flexor weakness is typically continuing to resolve during this period. Dr. Kazarian will monitor fusion progress with follow-up imaging.
- Avoid repetitive bending or heavy lifting until cleared by Dr. Kazarian
- No contact sports or strenuous recreational activities
- Continue physical therapy as prescribed
Bone Fusion and Full Recovery
Solid bone fusion generally occurs between three and six months after surgery, although full maturation of the fusion may continue for up to a year. As the fusion solidifies, you can gradually return to more demanding physical activities as approved by Dr. Kazarian. Most patients experience lasting relief from the leg pain and back symptoms that led to surgery. Your surgical team will continue to follow your progress with periodic check-ups and imaging to confirm successful fusion.
- Gradually increase activity level based on surgeon guidance
- Some patients may have permanent activity modifications depending on the number of levels fused
- Continue core strengthening exercises long-term to support the spine
Follow-Up Schedule
- 2 weeks after surgery: Incision check, wound healing assessment, and review of early recovery progress
- 6 weeks after surgery: Clinical evaluation of pain and neurological function, possible X-rays, discussion of return to driving and light work
- 3 months after surgery: X-rays to assess fusion progress, physical therapy progress review, and gradual return to more activities
- 6 to 12 months after surgery: Follow-up imaging to confirm solid fusion and final assessment of outcomes
When to Call Your Doctor
Contact our office immediately if you experience any of the following:
- Fever of 101.5°F (38.6°C) or higher, which may indicate an infection
- Increasing redness, warmth, swelling, or drainage from the incision site
- New or worsening leg pain, numbness, or tingling that was not present immediately after surgery
- Significant worsening of hip flexor weakness or new difficulty lifting your leg on the operative side
- New or worsening numbness across the front of the thigh that is progressing rather than improving
- Sudden severe back pain that is different from your typical post-operative discomfort
- Difficulty with bladder or bowel function, including inability to urinate or new incontinence
- Chest pain, shortness of breath, or calf swelling, which could indicate a blood clot
- Any fall or injury to the surgical area
Take this info home
Scan this QR code with your phone to save this page and review it at home. You can also share it with family members.
https://kazarian-surgery-portal.vercel.app/en/surgeries/lateral-interbody-fusion
Questions about your Lateral Lumbar Interbody Fusion?
Ask below and we’ll do our best to help. For urgent concerns, please call our office directly.
Have a question about your upcoming surgery? Type it below and we’ll find the answer for you.