Dr. Erick Kazarian, MD
NYU Langone Spine Surgery — Patient Information
Scan the QR code to view this page online →
Cervical Disc Replacement (CDR)
Cervical Disc Replacement Surgery
Cervical disc replacement, also known as artificial disc replacement or total disc arthroplasty, is a surgical procedure that removes a damaged or degenerated disc in the neck and replaces it with an artificial implant designed to mimic the natural movement of a healthy disc. Unlike traditional anterior cervical discectomy and fusion (ACDF), which permanently joins two vertebrae together, cervical disc replacement preserves motion at the treated spinal segment. This motion-preserving approach allows you to maintain a more natural range of movement in your neck after surgery.
One of the primary advantages of cervical disc replacement over spinal fusion is the potential to reduce stress on the discs above and below the treated level. When two vertebrae are fused, the adjacent segments must compensate for the lost motion, which over time can accelerate wear and degeneration at those neighboring levels. By preserving motion, an artificial disc distributes forces more naturally across the cervical spine, which may lower the likelihood of developing adjacent segment disease and reduce the need for additional surgeries in the future.
Cervical disc replacement is typically recommended for patients who have a herniated disc or degenerative disc disease at one or two levels in the neck that is causing nerve compression, resulting in symptoms such as arm pain, numbness, tingling, or weakness. Ideal candidates generally have healthy bone quality, no significant facet joint arthritis at the affected level, and no spinal instability. Dr. Kazarian will conduct a thorough evaluation, including advanced imaging studies, to determine whether cervical disc replacement is the best option for your specific condition.
Images & Diagrams
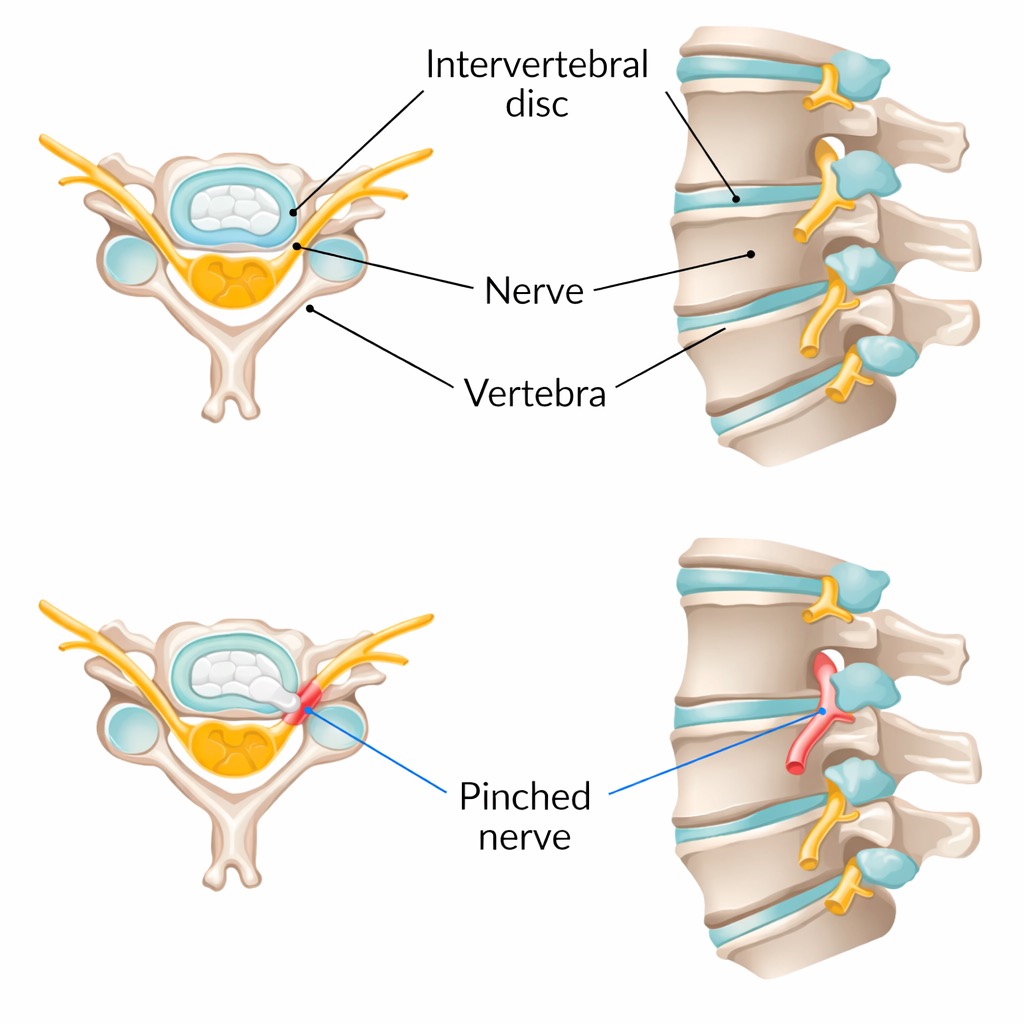
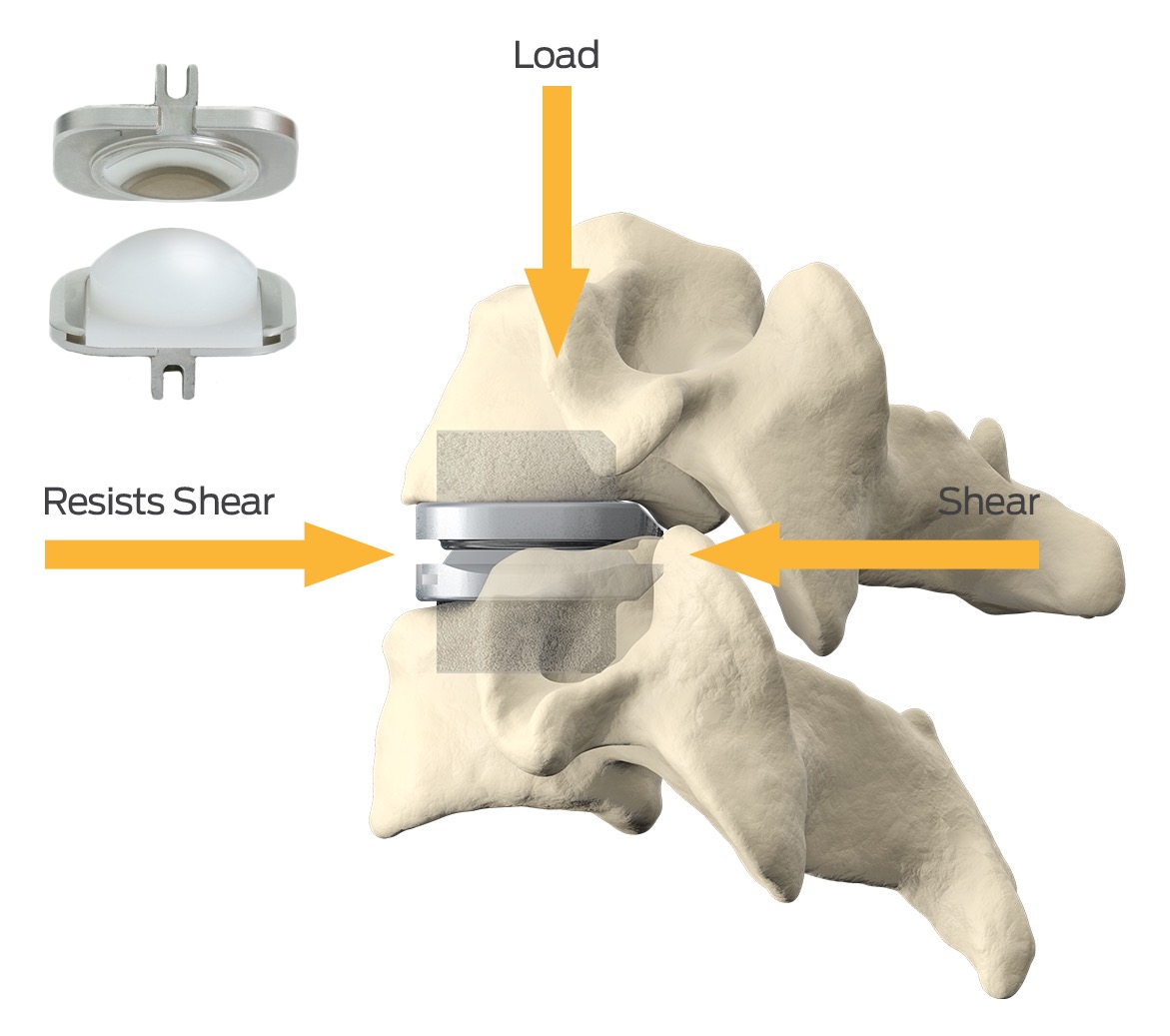
Pre-Operative Instructions
Carefully following these instructions before your cervical disc replacement helps ensure a safe procedure and supports the best possible outcome. Please contact our office if you have any questions or need clarification on any of these guidelines.
Review all current medications and supplements with Dr. Kazarian.
2 weeks before surgeryStop blood thinners (warfarin, aspirin, Plavix), NSAIDs (ibuprofen, naproxen), and herbal supplements (fish oil, vitamin E, ginkgo) as directed. GLP-1 receptor agonists (Ozempic, Wegovy, Mounjaro, Trulicity, Saxenda) must be stopped 7 days before surgery due to the risk of aspiration under anesthesia. Do not stop any medication without Dr. Kazarian's approval.
Obtain medical clearance from your primary care physician and any relevant specialists.
2-4 weeks before surgeryThis may include blood work, an EKG, and a health review. Bring clearance letters and your CPAP machine (if applicable) on surgery day.
Do not eat or drink anything after midnight the night before surgery.
After midnight the night before surgeryThis includes water, coffee, gum, and mints. You may take approved medications with a small sip of water.
The NYU perioperative team will call you the day before surgery with your arrival time.
Day of surgeryLocation: NYU Langone Kimmel Pavilion, 424 East 34th Street, Manhattan. Bring a valid photo ID, insurance card, and medication list.
Arrange for a responsible adult to drive you home and stay with you for 24 hours.
Arrange before surgery dayYou cannot drive after general anesthesia. Your driver should stay at the hospital during the procedure.
What to Expect on Surgery Day
Knowing what will happen before, during, and after your cervical disc replacement can help ease any anxiety and allow you to feel confident and prepared. Here is a step-by-step overview of your surgical experience.
Check-In and Pre-Operative Preparation
You will arrive at the hospital approximately two hours before your scheduled procedure. Our nursing team will verify your identity, review your medical history and current medications, and place an intravenous (IV) line. You will change into a hospital gown, and the surgical team will confirm the level of your spine being treated. Dr. Kazarian and anesthesiologist will visit you to review the plan, answer your questions, and ensure you feel comfortable before proceeding.
Anesthesia and Positioning
Cervical disc replacement is performed under general anesthesia, so you will be completely asleep and will not feel any pain during the procedure. Once the anesthesia takes effect, you will be carefully positioned on your back with your neck gently extended. The surgical team will use fluoroscopic X-ray imaging to confirm the precise spinal level before the first incision is made. Your vital signs, including heart rate, blood pressure, and oxygen levels, will be monitored continuously throughout the surgery.
Disc Removal and Implant Placement
Dr. Kazarian will make a small incision, typically one to two inches long, on the front of your neck. Working through natural tissue planes, the surgeon carefully accesses the cervical spine and removes the damaged disc along with any bone spurs or disc fragments that are pressing on the spinal cord or nerve roots. Once the disc space is fully prepared, the artificial disc implant is precisely positioned using real-time X-ray guidance to ensure optimal fit, alignment, and range of motion. The procedure typically takes approximately 60 to 90 minutes.
Closing the Incision
After the artificial disc is in place and proper positioning is confirmed, Dr. Kazarian carefully repositions the soft tissues and muscles back to their natural positions. The incision is closed with dissolvable stitches or surgical adhesive strips, and a small sterile dressing is applied. In some cases, a small drain may be placed near the incision to prevent fluid buildup; this is typically removed before you are discharged. The incision is made along a natural neck crease, so the resulting scar is typically thin and becomes barely noticeable over time.
Recovery Room
You will be moved to the post-anesthesia recovery area, where nurses will closely monitor your vital signs, neurological function, and comfort level as you wake up. You may experience mild soreness in your throat from the surgical approach, which is normal and temporary. Once you are fully alert and can swallow comfortably, you will be offered ice chips and clear liquids. You will then be moved to your private room for an overnight stay, where your care team will continue to monitor your recovery. Most patients are discharged the following morning.
Risks & Potential Complications
As with any surgical procedure, cervical disc replacement carries certain risks. While serious complications are uncommon, it is important that you understand the potential risks so you can make a fully informed decision. Dr. Kazarian will discuss these with you in detail during your consultation.
Infection
Any time an incision is made, there is a small risk of infection at the surgical site. Infections are uncommon with cervical spine surgery and are typically treatable with antibiotics when caught early. Signs of infection include increasing redness, swelling, warmth, or drainage from the incision, as well as fever.
Blood Loss
Some bleeding is expected during surgery. Significant blood loss requiring a transfusion is rare in cervical disc replacement procedures, but your surgical team is prepared to manage this if needed.
Cerebrospinal Fluid (CSF) Leak
The spinal cord is surrounded by a protective membrane that contains cerebrospinal fluid. In rare cases, this membrane can be nicked during surgery, causing a fluid leak. If this occurs, it is typically repaired during the procedure and may require a short period of additional bed rest to allow it to heal.
Adjacent Segment Disease
One of the advantages of disc replacement over fusion is that it preserves motion at the treated level, which may reduce stress on neighboring segments. However, adjacent segment disease can still occur over time, where disc levels above or below the implant develop new degeneration. This risk is generally considered lower with disc replacement compared to fusion.
Neurologic Injury
Although rare, there is a risk of injury to the spinal cord or nerve roots during surgery. This could result in symptoms ranging from mild numbness or tingling in the arms or hands to, in very rare cases, more significant weakness or paralysis. Dr. Kazarian uses specialized techniques and monitoring to minimize this risk.
Hardware Failure
The artificial disc implant is designed to be durable and long-lasting, but in rare cases the device may shift, wear, or malfunction. If this occurs, a revision surgery may be needed to reposition or replace the implant.
Autofusion (Heterotopic Ossification)
In some cases, new bone can form around the artificial disc over time, which may gradually limit the motion that the disc replacement was designed to preserve. This is called heterotopic ossification or autofusion. If it occurs, the artificial disc may function more like a fusion. While this reduces the motion-preserving benefit, many patients still experience good symptom relief.
Difficulty Swallowing (Dysphagia)
Because the surgery is performed through the front of the neck, it is common to experience some difficulty or discomfort when swallowing in the days and weeks after surgery. This is usually temporary and resolves on its own, though in rare cases it may persist longer.
Voice Changes (Dysphonia)
Some patients notice hoarseness or subtle changes in their voice after surgery. This is caused by temporary irritation of the recurrent laryngeal nerve, which runs near the surgical area. In most cases, the voice returns to normal within a few weeks, though rarely the changes may be longer lasting.
Cervical Hematoma
A hematoma is a collection of blood that can form near the incision after surgery. In the neck, a significant hematoma can cause swelling that may affect breathing or swallowing. This is a rare but serious complication that your care team monitors for closely in the hours after surgery. If it occurs, it may require a return to the operating room to drain the blood collection.
Need for Further Surgery
While cervical disc replacement has a high success rate, there is a possibility that additional surgery may be needed in the future. This could be due to implant issues, adjacent segment disease, autofusion, or recurrence of symptoms. Dr. Kazarian will discuss the likelihood of this based on your individual circumstances.
Recovery
Recovery from cervical disc replacement is generally faster than recovery from cervical fusion because the procedure preserves natural neck motion and does not require bone healing across a graft site. Most patients notice significant improvement in arm pain within the first few days to weeks after surgery. Neck soreness and mild throat discomfort from the surgical approach typically resolve within one to two weeks. While many patients return to light activities and desk work within two to four weeks, full recovery and return to all activities usually takes about three months. Dr. Kazarian will guide your recovery based on your individual progress at each follow-up visit.
Prescribed Medications
| Medication | Type | Dosage | Frequency | When to Take |
|---|---|---|---|---|
| Flexeril (cyclobenzaprine) | Muscle Relaxer | 5 mg | Every 6 hours as needed | Take for moderate to severe muscle spasm or pain |
| Tylenol (acetaminophen) | Pain Reliever | 500–1000 mg | Every 6 hours as needed | Take for mild pain |
| Tramadol | Semi-Narcotic Pain Reliever | 75 mg | Every 6 hours as needed | Take for moderate to severe pain not controlled by Tylenol or NSAIDs |
Always take medications exactly as prescribed by your surgeon. Do not combine pain medications without consulting your doctor.
Early Recovery
It is normal to experience neck soreness, throat discomfort, mild difficulty swallowing, and some hoarseness during the first several days. These symptoms are caused by the surgical approach through the front of the neck and typically improve steadily. Arm pain and neurological symptoms such as tingling or numbness often improve quickly as the pressure on the nerves has been removed. Most patients transition from prescription pain medication to over-the-counter options within seven to ten days and can resume light daily activities such as simple meals and short walks.
- Do not lift anything heavier than 15 pounds
- Do not drive or operate machinery while taking narcotic pain medication
- Avoid bending, twisting, or rotating your neck
- Keep your incision clean and dry — do not submerge in water (no baths, pools, or hot tubs)
- Take short, gentle walks several times a day to promote circulation
Progressing Recovery
By two to six weeks, most patients notice a significant reduction in neck and arm pain and can comfortably perform many of their usual daily activities. Dr. Kazarian may clear you to begin driving and return to sedentary or light-duty work. Physical therapy may be introduced during this period to help restore neck range of motion, strengthen supporting muscles, and improve posture. Because cervical disc replacement preserves motion, recovery is often faster than with fusion procedures.
- Do not lift anything heavier than 15 pounds
- Follow your physical therapy program as prescribed
- No high-impact activities, contact sports, or vigorous exercise
- Continue to avoid excessive neck bending, twisting, or extension
Full Recovery and Return to Activity
Most patients reach full recovery between three and six months after surgery. By this time, the artificial disc has integrated well with the surrounding vertebrae, and neck strength and flexibility should be near their optimal levels. Dr. Kazarian will evaluate your progress with follow-up imaging and clear you to return to all activities, including sports, heavy lifting, and physically demanding work. The artificial disc is designed to function for many years, and most patients enjoy long-lasting symptom relief and preserved neck motion.
- Follow any remaining activity guidelines provided by Dr. Kazarian
- Report any new or returning symptoms such as arm pain, numbness, or weakness
- Continue a regular neck strengthening and flexibility routine for long-term spinal health
Follow-Up Schedule
- First post-operative visit: 10 to 14 days after surgery for wound check and incision assessment
- Second follow-up: 6 weeks after surgery to evaluate healing, review imaging, and progress activity level
- Third follow-up: 3 months after surgery to assess spinal motion, symptom resolution, and functional recovery
- Fourth follow-up: 6 months after surgery with X-rays to evaluate implant position and disc motion
- Annual follow-up: Yearly visits may be recommended to monitor the long-term performance of the artificial disc
When to Call Your Doctor
Contact our office immediately if you experience any of the following:
- Fever above 101.5 degrees Fahrenheit that persists beyond the first 48 hours after surgery, or any fever accompanied by chills
- Increasing redness, swelling, warmth, or drainage from the incision, especially if the drainage is cloudy, yellowish, or has an unpleasant odor
- Difficulty breathing, swallowing, or a sensation of progressive swelling in the front of the neck, which could indicate a rare but serious post-operative hematoma
- New or worsening arm pain, numbness, tingling, or weakness that was not present before surgery or that returns after initially improving
- Sudden severe headache, changes in vision, or difficulty speaking, which require immediate emergency medical attention
- Chest pain, shortness of breath, or calf swelling and tenderness, which may indicate a blood clot and requires immediate medical evaluation
- Pain that is not controlled by your prescribed medications or that worsens significantly after an initial period of improvement
Take this info home
Scan this QR code with your phone to save this page and review it at home. You can also share it with family members.
https://kazarian-surgery-portal.vercel.app/en/surgeries/cervical-disc-replacement
Questions about your Cervical Disc Replacement (CDR)?
Ask below and we’ll do our best to help. For urgent concerns, please call our office directly.
Have a question about your upcoming surgery? Type it below and we’ll find the answer for you.